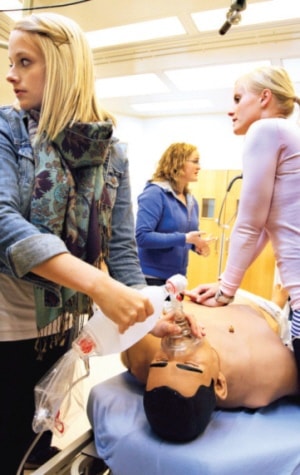
The halls of the Ponoka Hospital and Care Centre were full June 9, but not with patients - this time it was students.
There were 74 first - and second-year medical and nursing students who converged on the hospital to learn their curriculum in a rural setting. As most of them come from larger centres it gave them a chance to consider the idea of life in a small town as well as the scope of practice they would most likely be responsible for.
Bringing students to Ponoka is a project of the Alberta Rural Physician Action Plan (RPAP), whose goal is to assist doctors transition into a rural town and retain them. Cait Wills, RPAP communications co-ordinator, said the goal is to host four rural training days per year and she has yet to see negative feedback from anyone involved; students, nurses, and doctors show their interest in the program.
Students not only delve further into their profession, but they also see what it takes to practice in a small town. Hospital site chief, Dr. Brendan Bunting, said the scope of practice is different than a city. “You get to do everything from delivering a baby to fixing a broken arm.”
Doctors in larger centres also tend to specialize in certain areas, whereas in a town such as Ponoka, a doctor might have a patient the day they are born to the day that same patient gives birth.
“It’s really continuity of care. Our rush would be out of the long-term,” he stated.
There was one slight difference to last weekend’s training - the nursing students. There were 17 in the bachelor of nursing program at Mount Royal University, which is not typical practice. Rosemary Burness, medical students’ initiatives co-ordinator for RPAP, received requests from nurses to include nursing students in the rural training day. “Every town you go to the nursing students say, ‘Why don’t you have nurses in the class?’ RPAP is interested in a more multi-disciplinary focus.”
There are overlaps in first-and second-year medical education with nursing education. Elizabeth de Klerk, a medical student at the University of Calgary who is part of the university’s rural medicine interest group, said both medical and nursing students were able to have a better idea of each other’s work. “It’s easy to match nursing students with medical students right now because they’re in early stages of medical education.”
Since rural communities are not only short of doctors, but nurses as well, she feels it will help strengthen relationships between both groups. “It’s really important to work together.”
As all of the students are still learning, it is fairly clear there will not be a short-term fix to the issues Ponoka — and other rural towns — faces; one wing has been closed for some time and two doctors have recently left town.
David Kay, RPAP executive director, said there has been growth with doctors starting practices in rural Alberta; 1,888 expected for 2012 compared to 1,775 in 2011. Rural retention rates are relatively high. In 2004, there were 1,380 rural physicians and in 2010 to 2011 there were still 1,021 of those same physicians practicing in rural areas.
“We’re closing the gap in terms of the number of doctors in the province,” said Kay.
Schools are producing more physicians, overseas recruitment is up and doctors are staying in their jobs longer. “Where we seem to have issues is the distribution of those physicians.”
Kay said this is a worldwide issue, but the impact on a smaller community is more significant. He used an example of a small town with five newspaper reporters compared to a city with 50; if one of those reporters became unavailable the workload would increase. “It’s a pretty significant hole to fill.”
A loss of five reporters in the city would be significant but would not have the same impact as in a rural setting. “Just using that example in rural communities, the absence of one or two physicians in a smaller community where you don’t have the same critical mass as in a larger community can sometimes have a more significant impact.”
Kay feels the skills days give medical students a taste of rural Alberta and for those who enjoy the life, it may be an option after graduation.
Ponoka has its own doctor attraction and retention committee, which RPAP helped organize. Kay sees this as a more effective way to bring and keep physicians rather than with a reactive approach. When asked what he felt about paying doctors as an incentive to bring them to town Kay believed it is not the most effective method. Partly because doctors are paid fairly well. “We (Alberta) have one of the best physician agreements that are available as well as remuneration.”
He feels the better approach is to identify the needs of the doctors and their families. Money may not be as helpful as finding suitable short-term and long-term housing, or the spouse and children have specific activities they would hope to see in a rural town.
“Those tend to be much more effective and efficient ways of recruiting than financial incentives,” he explained.
Kay did not want to dismiss the financial incentive, but the committee should make a more “targeted approach.”
Dr. Izak van der Westhuizen also feels there are long-term benefits from the experience as students are not only eager to learn, but “there’s a lot of questions about rural living.”
“The thing we’re going to achieve is to create awareness among nursing and medical graduates,” he explained.
He also thought the opportunity nurses had from the learning could only bring about positive results.
“Over exposure is never harmful to anybody.”
Nursing student Laura Derhousoff said the day was an eye-opener into her medical training. “I’m strongly considering medical school now.”
Some universities have recently introduced the Rural Integrated Community Clerkship (RICC). Third-year medical students spend up to 36 months in a rural town and learn what it takes to be a rural physician. One of the instructors, Dawn Poisson, now in her last year of medical training, was able to give first-hand account of her experiences to the students of her experience at the Medical Centre in Ponoka.
“Everything that they (doctors) do, we get to do,” she said.
Poisson was worried her training would fall behind, but instead found she “took on more responsibility.”
Michelle Shewchuk, a registered nurse in Ponoka, said in a rural hospital there is a tendency to have well-rounded knowledge; when they have to deal with an issue, there may not necessarily be anyone else to take care of a patient’s needs. She feels the skills day was beneficial to everyone involved.
“This has been a great day. I like that they’re (students) excited,” she stated.
There were two STARS mobile training units; one of the stations had a flight paramedic, Manpreet Uppal, and Kirk Dobrowski, a community education leader for STARS. Uppal and Dobrowski had a hi-tech dummy, iStan, that is able to simulate almost any ailment imaginable. For this class, Uppal programmed a 53-year-old man having a heart attack. They could read vital signs on a screen, listen to his heart and even speak to iStan.
“He breathes, he talks, he has a pulse like you and I…I can make his tongue swell,” explained Uppal.
All the students were trained on how to administer injections, using an orange as their subject. They learned how to start an IV on a dummy arm and as they gained more confidence, on each other. They were shown birthing practices and how to monitor a baby’s progress. Bunting gave them a chance to practice suture skills on parts from pigs, which is slightly tougher than human skin, and van der Westhuizen demonstrated how to build and cut a cast.
The day was closed with a thank you barbecue hosted by Ponoka’s doctor retention committee and the next day students were given a tour of the Centennial Centre for Mental Health and Brain Injury and some of the programs it offers.